Blog
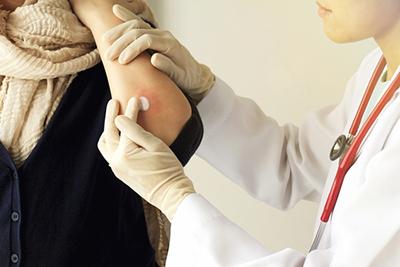
What To Know About Skin Cancer
- posted: Apr. 18, 2024
Skin cancer is one of the most common types of cancer and can be life-threatening if it isn’t treated at an early stage. Luckily, skin cancer is also highly preventable Read More
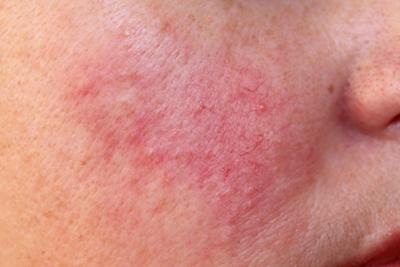
Rosacea: Understanding Triggers and Treatment Options for Managing Flare-Ups
- posted: Apr. 10, 2024
Your skin is a very important part of your overall physical appearance and attractiveness, so you will immediately notice any change in its color, texture, or new blemishes. One skin Read More
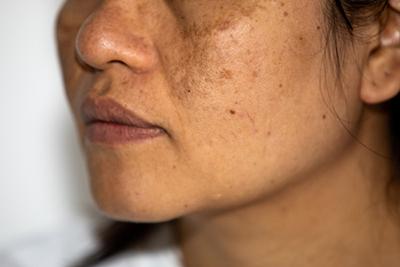
Mole Check: Importance of Regular Skin Exams for Early Detection
- posted: Apr. 03, 2024
Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or Read More
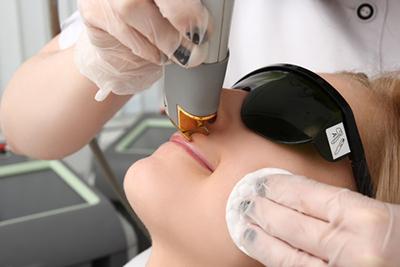
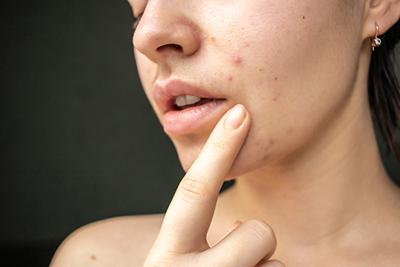
Benefits and Advantages of Laser Hair Removal
- posted: Apr. 01, 2024
Constant hair removal might feel like a chore, and you can deal with pain and irritation as your hair quickly grows back. When looking for hair removal treatments, you may Read More
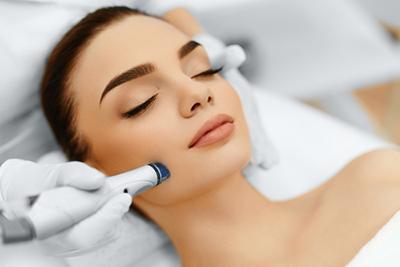
Understanding the Microdermabrasion Process
- posted: Mar. 19, 2024
What is Microdermabrasion? Microdermabrasion is a minimally invasive cosmetic procedure that exfoliates and removes the outermost layer of dead skin cells using a specialized device. This helps to stimulate cell turnover and Read More
What You Need To Know About Cosmetic Dermatology
- posted: Mar. 01, 2024
Cosmetic dermatology is focused on you looking your best. No matter what the aesthetic concern is, there is a procedure to help minimize the problem, so you can look great. Read More
Hormonal Acne: Causes, Diagnosis, and Treatment Options
- posted: Feb. 09, 2024
Acne is a skin condition that causes pimples, pustules, nodules, and other blemishes to appear on the skin, sometimes overnight. It is usually caused by an overproduction of oil as Read More
Cosmetic Dermatology: Exploring Non-Surgical Aesthetic Procedures
- posted: Feb. 01, 2024
Cosmetic dermatology focuses on enhancing the appearance of the skin, offering treatments aimed at refining, rejuvenating, and correcting various skin concerns. Cosmetic dermatology doesn't revolve around vanity. It boosts confidence Read More
Common Skin Conditions
- posted: Jan. 01, 2024
A dermatologist is a specialized medical professional focused on skin health. They're like skin detectives, trained extensively to diagnose, treat, and manage various skin, hair, and nail conditions. From acne Read More
Chemical Peels: Benefits, Risks, and Recovery
- posted: Dec. 15, 2023
Chemical Peels: Benefits, Risks, and Recovery Does your skin look dull and tired? Are you beginning to notice the early signs of aging, like fine lines and wrinkles? If so, it's Read More
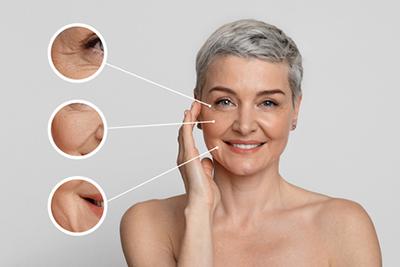
Common Signs of Aging Skin: Wrinkles, Fine Lines, and Texture Changes
- posted: Dec. 13, 2023
Looking Good Feeling Great in Indiana It is a fact of life that your skin changes as you age; how you take care of your skin when you are younger determines Read More
Managing Chronic Skin Conditions
- posted: Dec. 01, 2023
Chronic skin conditions can be embarrassing and uncomfortable. You may be able to manage a minor chronic skin condition on your own. For other chronic skin conditions, you can benefit Read More
Common Triggers of Rosacea Flare-Ups
- posted: Nov. 03, 2023
Rosacea is a chronic skin condition primarily affecting the face, often characterized by redness, visible blood vessels, and occasional pimples or bumps. Symptoms may vary, including facial flushing, persistent redness Read More
Rosacea: Understanding Triggers and Effective Treatment Approaches
- posted: Nov. 01, 2023
Rosacea is a chronic skin condition causing redness, visible blood vessels, and sometimes bumps on your face. Its exact cause isn't clear, but triggers like sunlight, stress, spicy food, and Read More
Hyperpigmentation: Causes and Solutions
- posted: Oct. 29, 2023
When dark marks and blemishes show up on the skin, it is usually due to a skin condition called hyperpigmentation. The marks can be either dark brown or black in Read More
Hormonal Acne: Causes and Treatment Approaches
- posted: Oct. 27, 2023
Dealing with acne is challenging, but understanding its various forms, identifying who's most susceptible, and knowing when to seek help from experts like Dr. Sonya Campbell Johnson at Dermatology Associates, Read More
Our Locations
TIPTON OFFICE
Medical Arts Building
Tipton, IN 46072, USA
Hours of Operation
7:00 am - 4:00 pm
8:00 am - 4:00 pm
7:00 am - 4:00 pm
7:00 am - 4:00 pm
7:00 am - 12:00 pm
Closed
Closed