Welcome to Expert Skin Cancer Treatment
Dermatology Associates, PC, a board‑certified dermatology group serving Indiana, specializes in comprehensive skin‑cancer care. Our team includes fellowship‑trained Mohs surgeons who act as surgeon, pathologist, and reconstructive specialist, ensuring precise, tissue‑sparing excisions. We prioritize personalized, compassionate care by counseling each patient on diagnosis, treatment options, and expected outcomes, and by tailoring plans to individual health status and cosmetic concerns. Advanced therapies such as Mohs micrographic surgery, targeted topical agents, and multidisciplinary reconstruction are routinely offered, providing the highest cure rates while preserving function and appearance. Our goal is to deliver expert, patient‑centered treatment that minimizes recurrence and maximizes quality of life.
Mohs Surgery: How It Works and Who Benefits
| Step | Description |
|---|---|
| 1 | Local anesthesia administered |
| 2 | Visible tumor debulked; 1–2 mm peripheral margin removed |
| 3 | Specimen mapped, frozen, sectioned, and stained |
| 4 | 100 % of peripheral and deep margins examined microscopically |
| 5 | Additional layers taken only from positive‑margin areas until clearance |
| 6 | Immediate reconstruction (suture, flap, graft, or secondary intention) |
Cure rates: 98‑99 % 5‑year cure for primary basal‑cell and squamous‑cell carcinomas; higher for low‑risk lesions. Minimal scarring due to tissue‑preserving approach.
 What does Mohs surgery stand for
What does Mohs surgery stand for
Mohs surgery is short for Mohs micrographic surgery, a precise, layer‑by‑layer technique developed by Dr. Frederic E. Mohs. Each thin tissue slice is examined under a microscope in real time, allowing the surgeon‑ act as pathologist and ensure that only cancer‑containing tissue is removed while preserving healthy skin.
Step‑by‑step layer‑by‑layer technique
- Local anesthesia is administered.
- The visible tumor is debulked and a 1–2 mm peripheral margin is removed.
- The specimen is mapped, frozen, sectioned, and stained.
- Microscopic examination of 100 % of peripheral and deep margins determines if cancer cells remain.
- Additional layers are taken only from areas with positive margins until all margins are clear.
- Immediate reconstruction (suturing, flap, graft, or secondary intention) follows clearance.
Cure rates and tissue preservation
Mohs achieves 5‑year cure rates of 98‑99 % for primary basal cell and squamous cell carcinomas, with even higher rates for low‑risk lesions. Because only cancerous tissue is excised, scarring is minimal and functional and cosmetic outcomes are superior to conventional excision.
What qualifies for Mohs surgery
Indications include high‑risk or recurrent basal cell and squamous cell carcinomas, tumors in cosmetically or functionally critical sites (face, ears, eyes, nose, lips, hands, feet, genitalia), lesions with ill‑defined borders, large or rapidly growing tumors, and immunosuppressed patients.
Why is Mohs surgery not used for melanoma
Melanoma often extends deeper than the superficial layers and requires wide margins plus sentinel‑node evaluation for accurate staging. Mohs’s layer‑by‑layer, epidermal‑focused approach cannot reliably assess depth or provide the immunohistochemical stains needed to identify atypical melanocytes; therefore, wide local excision remains the gold standard for melanoma.
What to Expect on the Day of Mohs Surgery
| Phase | Approx. Time | Key Details |
|---|---|---|
| Pre‑procedure | 30‑60 min | Medication hold (aspirin, ibuprofen, etc.), shower, no makeup, wear loose warm clothing, bring companion |
| Anesthesia | 5‑10 min | Local lidocaine injected; patient stays awake, pain‑free |
| Stage 1 (excision & mapping) | 15‑30 min | Tumor removed, tissue frozen, sectioned, stained |
| Microscopic review | 10‑20 min | Pathologist‑surgeon examines 100 % margins |
| Additional stages (if needed) | 15‑30 min each | Repeat until all margins clear |
| Reconstruction | 30‑90 min | Sutures, flap, graft, or secondary intention closure |
| Post‑op observation | 30‑60 min | Bandage applied, discharge instructions given |
Total visit: Typically 2‑5 hours; plan for a full‑day commitment.
 Pre‑procedure preparation and medication adjustments – Prior to the appointment, stop aspirin, ibuprofen, vitamin E, fish‑oil, and other herbal supplements 10‑14 days (and alcohol 48 hrs) to reduce bleeding. If you take blood‑thinners for a medical condition, discuss a safe pause with your surgeon. Shower, avoid makeup on facial lesions, wear loose, warm clothing, and bring a companion for transport and support. Pack snacks, a book or tablet, and your regular medications (e.g., antihypertensives, diabetes pills) because the process can occupy most of the day.
Pre‑procedure preparation and medication adjustments – Prior to the appointment, stop aspirin, ibuprofen, vitamin E, fish‑oil, and other herbal supplements 10‑14 days (and alcohol 48 hrs) to reduce bleeding. If you take blood‑thinners for a medical condition, discuss a safe pause with your surgeon. Shower, avoid makeup on facial lesions, wear loose, warm clothing, and bring a companion for transport and support. Pack snacks, a book or tablet, and your regular medications (e.g., antihypertensives, diabetes pills) because the process can occupy most of the day.
Typical duration and day‑long appointment – Mohs surgery is performed in stages; each thin tissue layer is frozen, sectioned, and examined (15‑30 min per layer). Most cases require 1‑3 stages, making the total visit 2‑5 hours, and patients should plan for a full‑day commitment.
Local anesthesia and patient comfort – Only local anesthetic (usually lidocaine) is used, so you stay awake but feel no pain. The surgeon acts as pathologist and reconstructive specialist, allowing immediate margin assessment and same‑day wound closure.
Post‑operative care and recovery timeline – After tumor clearance, the wound may be closed with sutures, flaps, or grafts. Expect mild pain, swelling, and a bandage for 5‑7 days; over‑the‑counter analgesics suffice. Follow‑up visits at 1‑2 weeks monitor healing and plan future skin checks.
What I wish I knew before Mohs surgery? – I didn’t realize the procedure can last 5‑6 hours, that smoking cessation, medication stops, and a full day of waiting are essential, and that the goal is complete cancer removal with maximal tissue preservation, resulting in cure rates >98 % and minimal scarring.
What is the average cost of skin cancer removal? – Mohs surgery typically costs $1,500‑$5,000 total, with each stage $500‑$1,500. Reconstruction (flap or graft) adds $2,000‑$5,000. Most insurance plans cover the majority, leaving a modest out‑of‑pocket amount.
Is Mohs surgery considered a major surgery? – It is classified as a minor outpatient procedure performed under local anesthesia, though complexity varies with tumor size and location.
Site‑Specific Considerations: The Nose and Other High‑Risk Areas
| Defect Size | Preferred Reconstruction | Key Points |
|---|---|---|
| ≤5 mm (small) | Primary closure | Direct suturing; minimal scar, preserves nasal valve function |
| 5‑15 mm (moderate) | Local flap (e.g., bilobed, melolabial) | Uses adjacent tissue; maintains contour and aesthetic units |
| >15 mm or complex contour | Regional flap (forehead or nasolabial) | Robust blood supply; excellent match for nasal skin texture |
| Deep full‑thickness loss | Full‑thickness skin graft or composite graft | Requires donor site; may need secondary revision for contour |
| High‑risk functional area (e.g., nasal valve) | Staged reconstruction with cartilage grafts | Preserves airway patency; may combine with flap for lining |
Outcome: Cure rates 98‑99 % for nasal BCC/SCC; reconstruction tailored to preserve function and aesthetics.
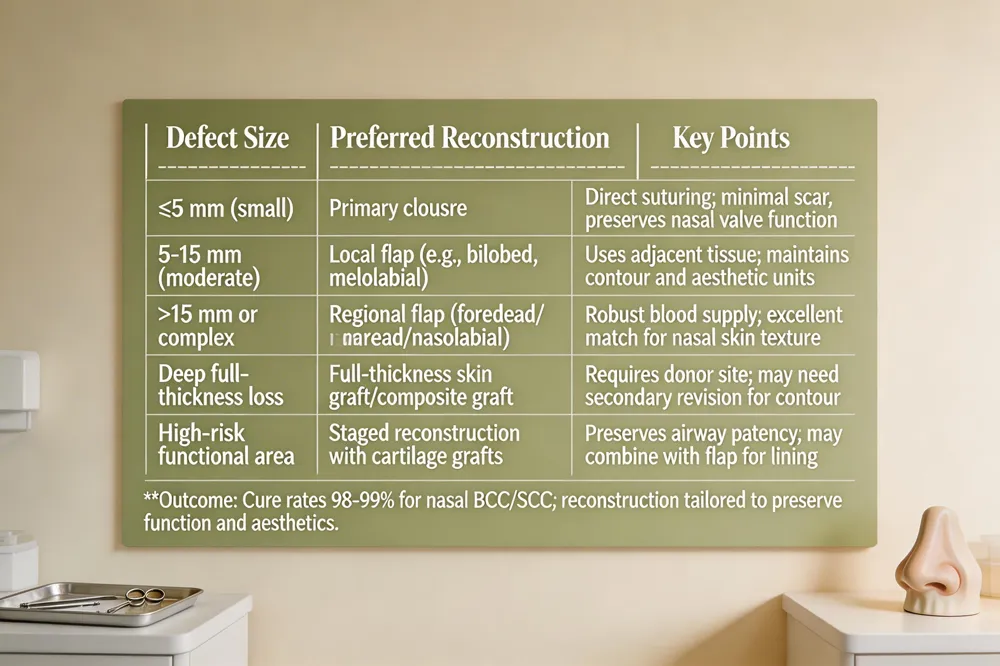 The nose presents a unique anatomical challenge for skin‑cancer surgery. Its cartilaginous framework, thin skin, and complex contours demand precise removal of tumor while preserving critical structures such as the nasal valve and external aesthetic units. Mohs micrographic surgery meets these demands by excising thin, mapped layers of tissue and examining 100 % of the peripheral and deep margins in real time. This step‑by‑step approach yields cure rates of 98‑99 % for basal cell and squamous cell carcinomas on the nose and minimizes unnecessary loss of healthy skin.
The nose presents a unique anatomical challenge for skin‑cancer surgery. Its cartilaginous framework, thin skin, and complex contours demand precise removal of tumor while preserving critical structures such as the nasal valve and external aesthetic units. Mohs micrographic surgery meets these demands by excising thin, mapped layers of tissue and examining 100 % of the peripheral and deep margins in real time. This step‑by‑step approach yields cure rates of 98‑99 % for basal cell and squamous cell carcinomas on the nose and minimizes unnecessary loss of healthy skin.
After clear margins are achieved, reconstruction is tailored to the defect’s size and location. Options include primary closure for small wounds, local flaps that borrow adjacent tissue to restore shape, and skin grafts for larger areas. Advanced techniques such as nasolabial or forehead flaps can rebuild the contour of the nasal tip or alae, delivering functional and cosmetic results that closely match the original anatomy.
Mohs surgery on nose: Mohs micrographic surgery is the gold‑standard treatment for basal cell, squamous cell and other skin cancers on the nose because it removes cancer layer by layer while preserving as much healthy tissue as possible. During the outpatient procedure the area is numbed, the surgeon excises ultra‑thin strips of skin, and each strip is examined under a microscope in real time until no cancer cells remain, resulting in cure rates up to 99 %. Because the nose has complex contours and vital structures, our board‑certified Mohs surgeons carefully plan reconstruction—using flaps, grafts or primary closure—to minimize scarring and maintain the natural shape of the nose. Common side effects are limited to temporary swelling, tenderness, or a small, well‑concealed scar that typically fades over months. Most patients resume normal activities within a week and appreciate the confidence of knowing their skin cancer has been completely removed with minimal cosmetic impact.
Emerging and Complementary Skin Cancer Treatments
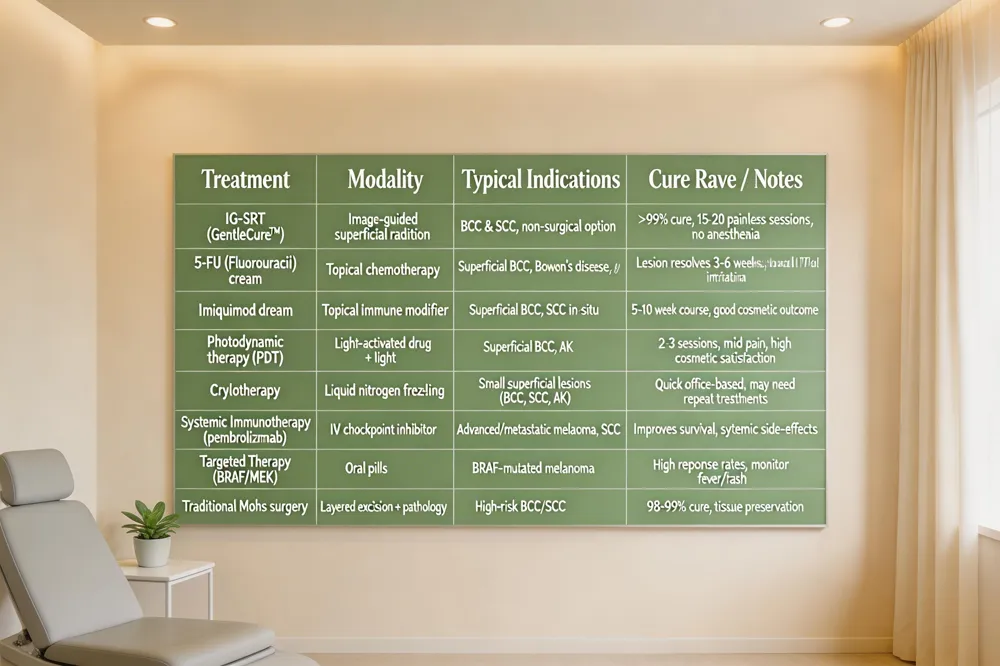
| Treatment | Modality | Typical Indications | Cure Rate / Notes |
|---|---|---|---|
| IG‑SRT (GentleCure™) | Image‑guided superficial radiation | BCC & SCC, patients preferring non‑surgical option | >99 % cure, 15‑20 painless sessions, no anesthesia |
| 5‑FU (Fluorouracil) cream | Topical chemotherapy | Superficial BCC, Bowen’s disease, actinic keratoses | Lesion resolves in 3‑6 weeks; local irritation common |
| Imiquimod cream | Topical immune response modifier | Superficial BCC, SCC in‑situ | 5‑10 week course; good cosmetic outcome |
| Photodynamic therapy (PDT) | Light‑activated drug + light exposure | Superficial BCC, actinic keratoses | 2‑3 sessions; mild pain, high cosmetic satisfaction |
| Cryotherapy | Liquid nitrogen freezing | Small superficial lesions (BCC, SCC, AK) | Quick, office‑based; may require repeat treatments |
| Systemic immunotherapy (e.g., pembrolizumab) | Intravenous checkpoint inhibitor | Advanced/metastatic melanoma, SCC | Improves survival; significant systemic side‑effects |
| Targeted therapy (BRAF/MEK inhibitors) | Oral pills | BRAF‑mutated melanoma | High response rates; monitor for fever, skin rash |
| Traditional Mohs surgery | Layer‑by‑layer excision with intra‑operative pathology | High‑risk or cosmetically sensitive BCC/SCC | 98‑99 % cure, tissue preservation |
 What is the new alternative to Mohs surgery?
The newest non‑surgical option for treating basal and squamous cell carcinomas is Image‑Guided Superficial Radiation Therapy (IG‑SRT), marketed under the brand name GentleCure™. IG‑SRT delivers low‑dose, precisely targeted X‑ray energy to cancer cells while sparing surrounding healthy tissue, allowing the skin to heal naturally without incisions or sutures. Clinical studies show cure rates exceeding 99 % for these skin cancers, comparable to or better than traditional Mohs surgery, but with no anesthesia, scarring, or prolonged wound care. Treatment consists of 15‑20 short, painless sessions over several weeks, enabling patients to resume normal activities immediately.
What is the new alternative to Mohs surgery?
The newest non‑surgical option for treating basal and squamous cell carcinomas is Image‑Guided Superficial Radiation Therapy (IG‑SRT), marketed under the brand name GentleCure™. IG‑SRT delivers low‑dose, precisely targeted X‑ray energy to cancer cells while sparing surrounding healthy tissue, allowing the skin to heal naturally without incisions or sutures. Clinical studies show cure rates exceeding 99 % for these skin cancers, comparable to or better than traditional Mohs surgery, but with no anesthesia, scarring, or prolonged wound care. Treatment consists of 15‑20 short, painless sessions over several weeks, enabling patients to resume normal activities immediately.
Skin cancer treatment cream Topical fluorouracil (5‑FU) cream is an FDA‑approved chemotherapy that dermatologists use to treat superficial skin cancers such as basal cell carcinoma, Bowen’s disease, and actinic keratoses that could progress to squamous cell carcinoma. The medication works by interfering with DNA synthesis in rapidly dividing cancer cells, causing the lesions to become red, inflamed, and eventually peel off as healthy skin regrows. Patients typically apply a thin layer to the affected area once or twice daily for 3‑6 weeks, following the exact schedule prescribed by their dermatologist and avoiding airtight dressings unless instructed otherwise. Common side effects include localized redness, swelling, crusting, and heightened sun sensitivity, so sun protection and gentle skin care are essential during treatment.
8 types of skin cancer treatment The primary treatment options for skin cancer include:
- Surgery – ranging from traditional excision to Mohs micrographic surgery, which removes the tumor with a margin of healthy tissue.
- Radiation therapy – both external beam and superficial radiation, which delivers targeted energy to destroy cancer cells while sparing surrounding skin.
- Topical chemotherapy – agents like 5‑FU or imiquimod applied directly to superficial lesions.
- Curettage‑electrodessication – scraping and cauterizing lesions for superficial tumors.
- Photodynamic therapy – a light‑activated drug selectively kills malignant cells after a brief incubation period.
- Cryotherapy – freezing lesions with liquid nitrogen.
- Systemic therapies – immunotherapy, targeted therapy (e.g., BRAF/MEK inhibitors), and, in selected cases, chemotherapy for advanced disease.
- Image‑Guided Superficial Radiation Therapy (IG‑SRT) – a precise, non‑invasive radiation option (GentleCure™) that rivals Mohs surgery in cure rates.
Skin cancer treatment face Treating skin cancer on the face begins with an accurate biopsy and, if needed, staging to determine depth and spread. For most basal‑cell and squamous‑cell lesions, Mohs micrographic surgery is the preferred option because it removes the cancer layer‑by‑layer while sparing healthy tissue, resulting in high cure rates and minimal scarring. Smaller or superficial tumors can be managed with cryotherapy, curettage with electrodessication, or topical chemotherapy such as 5‑fluorouracil, which are effective and preserve facial contour. When surgery is not ideal, photodynamic therapy or laser ablation offers a non‑invasive alternative that targets cancer cells with light‑activated drugs. Advanced or high‑risk facial melanomas may require a multidisciplinary approach that combines surgery with radiation, targeted therapy, or immunotherapy to ensure comprehensive control.
Skin cancer treatment melanoma Melanoma is primarily treated with surgery, which removes the tumor and a margin of healthy tissue to reduce the risk of recurrence; for lesions on the face or other cosmetically sensitive areas, a plastic surgeon may perform reconstructive techniques such as skin grafts. When the cancer has spread to regional lymph nodes or distant sites, additional therapies—radiation, targeted‑therapy drugs that block specific genetic mutations, and immunotherapy that activates the immune system—are often employed to control disease and improve survival. Chemotherapy may be used for advanced cases, though it is generally less effective than newer targeted or immune‑based treatments. Your dermatology team will tailor a multidisciplinary plan based on the melanoma’s stage, location, and your overall health, and will discuss potential side effects and follow‑up monitoring.
Your Local Dermatology Experts and Access to Care
| Location | Address | Contact | Services |
|---|---|---|---|
| Dermatology Center of Indiana – Greenwood | 2800 South State Rd., Suite 135, Greenwood, IN | 317‑555‑1234 | General dermatology, Mohs surgery, aesthetics, laser |
| DCI – Plainfield | 2155 E Main St., Plainfield, IN 46168 | 317‑838‑9911 (Dr. Scott T. Guenthner) | Acne, eczema, skin cancer, Mohs surgery |
| IU Health – Indianapolis (Female dermatologist) | 931 E 86th St., Ste 104, Indianapolis, IN | 317‑555‑5678 (Dr. Janelle S. Nassim) | Medical, cosmetic, surgical dermatology |
| Ascension St. Vincent – Indianapolis (Female dermatologist) | 1234 N Meridian St., Indianapolis, IN | 317‑555‑9012 (Dr. Sonya F. Johnson) | Mohs, laser, cosmetic procedures |
| Dermatology, Inc. – Avon | 10465 E County Rd., 100 N, Avon, IN | 317‑555‑3456 (Dr. Robert H. Huff) | Skin‑cancer treatment, aesthetics |
| IU Health Dermatology – Avon | 1115 N Ronald Reagan Pkwy., Suite 348, Avon, IN | 317‑555‑7890 | Comprehensive dermatology, Mohs surgery |
| Medicaid‑accepting clinic | IU Health Dermatology downtown, Indianapolis, IN | 317‑555‑6543 | General dermatology, skin‑cancer care (Medicaid accepted) |
2‑week rule: Referral for suspicious skin lesion → specialist appointment within 14 days.
 The dermatology center of Indiana
The dermatology center of Indiana
Dermatology Associates, PC operates the Dermatology Center of Indiana (DCI) at 2800 South State Rd., Suite 135, Greenwood, IN. The team includes board‑certified dermatologists such as Dr. Andrew J. Scripture and Dr. Shayna Gordon, offering general dermatology, Mohs micrographic surgery, medical aesthetics, and laser therapies with flexible weekday hours.
Dermatologist Plainfield Indiana
In Plainfield, DCI’s office at 2155 E Main St. (IN 46168) provides comprehensive skin care. Dr. Scott T. Guenthner, MD, leads a skilled staff treating acne, eczema, skin cancer, and performing Mohs surgery. Appointments are scheduled by calling 317‑838‑9911.
Female dermatologist Indianapolis
Two board‑certified female dermatologists practice in Indianapolis: Dr. Janelle S. Nassim, MD at IU Health, and Dr. Sonya F. Johnson, MD at Ascension St. Vincent and Dermatology Associates, PC (931 E 86th St Ste 104). Both offer medical, cosmetic, and surgical services, including Mohs surgery.
Dermatologist Avon Indiana
Avon residents can see Dr. Robert H. Huff, MD, FAAD at Dermatology, Inc. (10465 E County Rd 100 N) and the IU Health Dermatology Avon clinic (1115 N Ronald Reagan Pkwy, Suite 348) for comprehensive skin‑cancer and aesthetic care.
Best dermatologist in Indianapolis
Dermatology Associates, PC, led by Dr. Guenthner, is recognized as Indianapolis’s top practice, earning the Indianapolis Monthly Top Doctor Award and Angie’s List Super Service Award. It offers full‑service dermatology, Mohs surgery, and advanced cosmetic procedures across two convenient locations.
Dermatologist in Indianapolis that accepts Medicaid
Medicaid‑accepting options include Dr. Anna Chacon, MD (listed on Zocdoc) and IU Health Dermatology downtown, both providing medical and surgical skin care. Verify coverage via the Indiana Medicaid Provider Directory.
What is the 2‑week rule for skin cancer?
The 2‑week rule mandates that any patient with a lesion suspicious for skin cancer be seen by a specialist within 14 days of referral. Prompt assessment under this fast‑track pathway improves early detection and treatment outcomes.
Your Path to Clear, Healthy Skin
At Dermatology Associates, PC you will receive expert care from board‑certified Mohs surgeons who act as surgeon, pathologist, and reconstructive specialist in a single visit. Our clinic offers Mohs micrographic surgery—the gold‑standard for basal cell and squamous cell carcinomas in cosmetically sensitive areas—as well as alternative treatments such as excision, cryotherapy and radiation for cases where Mohs is not indicated. We prioritize patient education, providing clear pre‑procedure instructions, real‑time margin assessment results, and detailed post‑operative wound‑care guidance. Follow‑up appointments are scheduled to monitor healing, detect recurrence early, and reinforce sun‑protection habits, ensuring lasting skin health and quality of life for you.
