Why Understanding Skin Infections Matters
Skin infections affect millions annually, causing pain, itching, swelling, and, in severe cases, systemic illness that can impair daily activities and lower quality of life. Dermatologists play a critical role by distinguishing bacterial, fungal, and viral etiologies through clinical examination, skin scrapings, cultures, and PCR testing, allowing targeted therapy and preventing complications such as scarring or secondary infection. Bacterial infections—like cellulitis, impetigo, and MRSA—require antibiotics; fungal infections (athlete’s foot, ringworm, candidiasis) demand antifungal agents; viral conditions (herpes simplex, shingles, warts, molluscum) are managed with antivirals or procedural interventions. Accurate diagnosis and prompt, appropriate treatment are essential for rapid recovery and infection control.
Identifying the Culprit: Bacterial vs Fungal vs Viral Skin Infections
Quick Comparison Table
| Feature | Bacterial | Fungal | Viral |
|---|---|---|---|
| Typical lesion | Warm, red, swollen, may ooze pus or honey‑colored crusts (e.g., impetigo, cellulitis) | Itchy, well‑defined circular/ring‑shaped patches with raised scaly border (tinea) or moist plaques (candidiasis) | Vesicles, dome‑shaped papules, or painful band‑like rash following a dermatome (e.g., shingles) |
| Common examples | Staphylococcus aureus (incl. MRSA), Streptococcus pyogenes | Tinea corporis, Tinea pedis, Candidiasis | HSV‑1/2, VZV, HPV, Molluscum contagiosum |
| Systemic signs | Fever, chills, rapid expansion, pain | Usually localized itching; may have mild fever if extensive | Fever, fatigue, malaise possible; often with prodromal symptoms |
| Red‑flag signs | Rapid spread, increasing pain, fever, failure to improve with OTC | Expanding border, severe itching, secondary bacterial infection | Painful dermatomal rash, fever, vesicle rupture with crusting |
| Diagnostic tools | Swab culture, PCR, Gram stain | KOH prep, fungal culture, PCR | PCR, Tzanck smear, viral culture |
| First‑line treatment | Topical or oral antibiotics (e.g., bacitracin, dicloxacillin) | Topical antifungals (clotrimazole, terbinafine) | Antivirals (acyclovir, valacyclovir) or lesion‑specific therapy |
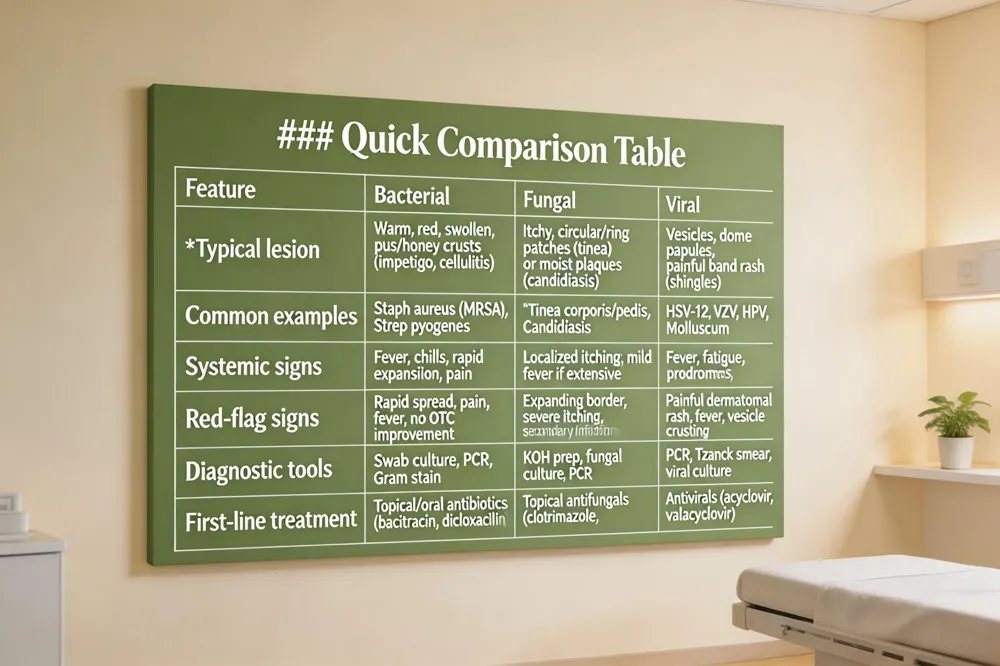 Key clinical differences help separate bacterial, fungal, and viral skin infections. Bacterial lesions are usually warm, red, swollen, may ooze pus or form honey‑colored crusts (e.g., impetigo, cellulitis) and can spread rapidly. Fungal infections appear as itchy, well‑defined circular or ring‑shaped patches with a raised, scaly border, thriving in warm, moist areas such as the feet, groin, or skin folds. Viral infections generate vesicles, dome‑shaped papules, or a painful, band‑like rash that follows a dermatome (e.g., shingles) and may be accompanied by systemic symptoms like fever or fatigue.
Key clinical differences help separate bacterial, fungal, and viral skin infections. Bacterial lesions are usually warm, red, swollen, may ooze pus or form honey‑colored crusts (e.g., impetigo, cellulitis) and can spread rapidly. Fungal infections appear as itchy, well‑defined circular or ring‑shaped patches with a raised, scaly border, thriving in warm, moist areas such as the feet, groin, or skin folds. Viral infections generate vesicles, dome‑shaped papules, or a painful, band‑like rash that follows a dermatome (e.g., shingles) and may be accompanied by systemic symptoms like fever or fatigue.
Diagnostic tools include a visual exam supplemented by skin scrapings for KOH preparation, cultures, or PCR testing to confirm the organism. Early identification of red‑flag signs—rapid expansion, increasing pain, fever, chills, or failure to improve with over‑the‑counter care—warrants urgent dermatologic evaluation.
How to tell if an infection is viral, bacterial, or fungal? The lesion’s texture (blister vs. pustule vs. scaly plaque), pattern of spread, and presence of systemic symptoms guide initial differentiation, but definitive diagnosis often requires a swab, culture, or PCR.
When to worry about a skin infection? Seek care if redness spreads outward in streaks, if fever or malaise develop, if pus or foul drainage appears, or if the rash persists despite proper home care—especially in diabetes, immunosuppression, or older age.
Bacterial skin infection causes Entry of pathogenic bacteria (Staphylococcus aureus, including MRSA, or Streptococcus pyogenes) through cuts, abrasions, hair‑follicle openings, or contaminated surfaces, combined with host factors such as eczema, diabetes, or immune compromise, initiates infection.
Fungal Skin Infections: Symptoms, Causes, and Treatment Strategies
Common Fungal Infections & Management
| Infection | Typical Site | Presentation | First‑line topical | When to consider oral therapy |
|---|---|---|---|---|
| Tinea corporis (ringworm) | Trunk, limbs | Red, circular, scaly patch with raised border | Clotrimazole 1% BID 2‑4 wks | Extensive, recurrent, or >5 cm lesions |
| Tinea pedis (athlete’s foot) | Between toes | Macerated, peeling skin, itching | Terbinafine 1% BID 2‑4 wks | Involvement of plantar surface or nail |
| n | Tinea cruris (jock‑itch) | Groin, inner thighs | Moist, erythematous, itchy rash | Miconazole 2% BID 2‑4 wks |
| Candidiasis | Skin folds, mucous membranes | Red, moist patches with satellite lesions | Nystatin or clotrimazole cream BID 2‑4 wks | Systemic signs or refractory cases |
| Onychomycosis | Nails | Thickened, discolored, brittle nails | Topical efinaconazole or tavaborole | Oral terbinafine/itraconazole for >50 % nail involvement |
Nutritional note: Vitamin D, vitamin A, zinc, and iron deficiencies can impair barrier function; supplementation may aid prevention.
 Fungal skin infections commonly present as itchy, red, scaly patches that may form circular, ring‑shaped lesions with a raised border (tinea corporis) or moist, cracked areas in skin folds (candidiasis). Blisters, fine scales, and swelling can accompany the rash, especially after sweating or friction.
Fungal skin infections commonly present as itchy, red, scaly patches that may form circular, ring‑shaped lesions with a raised border (tinea corporis) or moist, cracked areas in skin folds (candidiasis). Blisters, fine scales, and swelling can accompany the rash, especially after sweating or friction.
Risk factors that promote overgrowth include warm, moist environments (tight clothing, sweaty feet, skin folds), obesity, diabetes, recent broad‑spectrum antibiotics, hormonal changes, and immunosuppression. Maintaining dry, breathable skin reduces fungal proliferation.
First‑line therapy is topical antifungals such as clotrimazole, terbinafine, or miconazole applied twice daily for 2‑4 weeks, even after symptoms improve. Extensive, recurrent, or nail infections require oral agents (terbinafine, itraconazole, fluconazole) with liver‑function monitoring. Avoid over‑the‑counter steroid‑containing creams, as they can worsen infection.
Nutritional status influences susceptibility: deficiencies in vitamin D, vitamin A, zinc, and iron impair barrier integrity and immune defenses, increasing infection risk. A balanced diet, adequate sunlight exposure, and supplementation when needed support skin health.
FAQ
- Fungal skin infection symptoms: itching, redness, scaling, ring‑shaped rash, blisters, moist patches.
- What causes fungal infection in private parts?: Candida overgrowth triggered by warmth, moisture, tight clothing, antibiotics, diabetes, hormonal shifts, and immune compromise.
- Fungal skin infection treatment: topical antifungals for mild disease; oral antifungals for extensive or nail disease; keep skin dry and avoid steroid mixtures.
- What kills a fungal infection on skin?: Fungicidal or fungistatic agents—prescription‑strength creams (terbinafine, clotrimazole) and oral tablets (itraconazole, fluconazole).
- Which vitamin deficiency causes fungal infection?: Low vitamin D, vitamin A, zinc, or iron weakens antimicrobial defenses, predisposing to infection.
Viral Skin Infections: Recognizing, Managing, and Preventing Spread
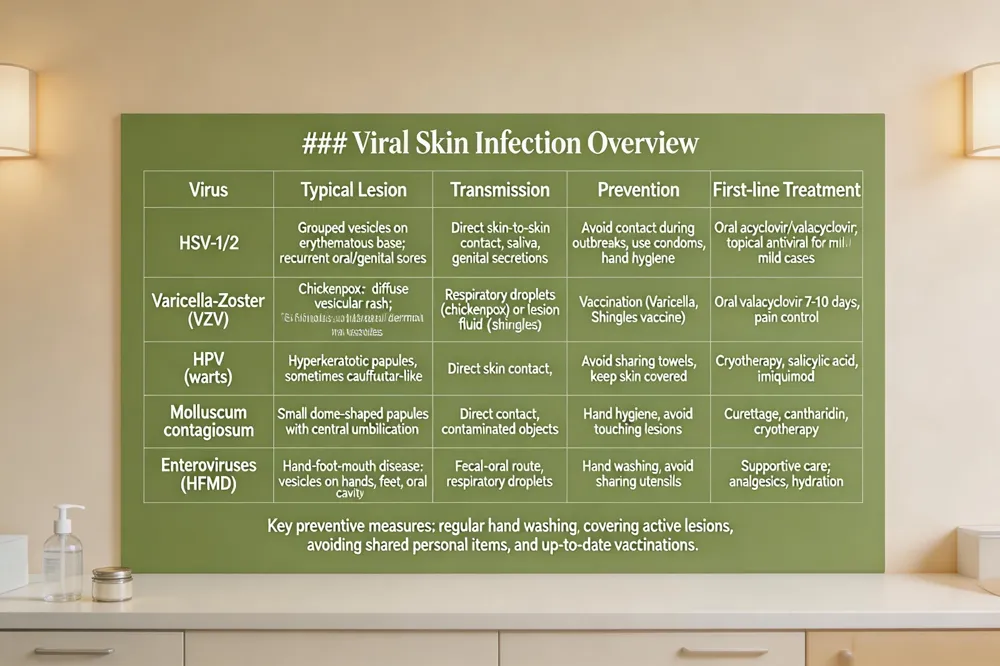
Viral Skin Infection Overview
| Virus | Typical Lesion | Transmission | Prevention | First‑line Treatment |
|---|---|---|---|---|
| HSV‑1/2 | Grouped vesicles on erythematous base; recurrent oral/genital sores | Direct skin‑to‑skin contact, saliva, genital secretions | Avoid contact during outbreaks, use condoms, hand hygiene | Oral acyclovir/valacyclovir; topical antiviral for mild cases |
| Varicella‑Zoster (VZV) | Chickenpox: diffuse vesicular rash; Shingles: unilateral dermatomal vesicles | Respiratory droplets (chickenpox) or lesion fluid (shingles) | Vaccination (Varicella, Shingles vaccine) | Oral valacyclovir 7‑10 days; pain control |
| HPV (warts) | Hyperkeratotic papules, sometimes cauliflower‑like | Direct skin contact, fomites | Avoid sharing towels, keep skin covered | Cryotherapy, salicylic acid, imiquimod |
| Molluscum contagiosum | Small dome‑shaped papules with central umbilication | Direct contact, contaminated objects | Hand hygiene, avoid touching lesions | Curettage, cantharidin, cryotherapy |
| Enteroviruses (HFMD) | Hand‑foot‑mouth disease: vesicles on hands, feet, oral cavity | Fecal‑oral route, respiratory droplets | Hand washing, avoid sharing utensils | Supportive care; analgesics, hydration |
Key preventive measures: regular hand washing, covering active lesions, avoiding shared personal items, and up‑to‑date vaccinations.
 In the United States the most common skin‑related viruses are herpes simplex (HSV‑1 and HSV‑2), varicella‑zoster (VZV, causing chickenpox and shingles), human papillomavirus (HPV w warts), and molluscum contagiosum virus. These infections typically appear as red or pink patches with vesicles, papules, or dome‑shaped bumps; herpes lesions cluster as grouped vesicles on an erythematous base, shingles follows a unilateral dermatomal pattern, warts are hyperkeratotic papules, and molluscum shows central umbilication. Children are especially prone to hand‑foot‑mouth disease, chickenpox, and molluscum, which spread via direct skin contact or shared items. Most viral skin infections are contagious—herpes spreads through saliva or genital secretions, VZV through respiratory droplets and lesion fluid, and molluscum by touching lesions or contaminated surfaces. Prevention relies on hand hygiene, avoiding sharing towels or clothing, and covering active lesions; vaccination against varicella‑zoster significantly reduces shingles risk. Treatment is virus‑specific: oral acyclovir, valacyclovir, or famciclovir for HSV and VZV; topical salicylic acid, cryotherapy, or immunomodulators for HPV warts; and curettage or cantharidin for molluscum. Supportive care—cool compresses, antihistamines, and moisturizers—relieves symptoms while the immune system clears the pathogen. Prompt dermatologic evaluation ensures accurate diagnosis, appropriate antiviral or procedural therapy, and education on contagion control.
In the United States the most common skin‑related viruses are herpes simplex (HSV‑1 and HSV‑2), varicella‑zoster (VZV, causing chickenpox and shingles), human papillomavirus (HPV w warts), and molluscum contagiosum virus. These infections typically appear as red or pink patches with vesicles, papules, or dome‑shaped bumps; herpes lesions cluster as grouped vesicles on an erythematous base, shingles follows a unilateral dermatomal pattern, warts are hyperkeratotic papules, and molluscum shows central umbilication. Children are especially prone to hand‑foot‑mouth disease, chickenpox, and molluscum, which spread via direct skin contact or shared items. Most viral skin infections are contagious—herpes spreads through saliva or genital secretions, VZV through respiratory droplets and lesion fluid, and molluscum by touching lesions or contaminated surfaces. Prevention relies on hand hygiene, avoiding sharing towels or clothing, and covering active lesions; vaccination against varicella‑zoster significantly reduces shingles risk. Treatment is virus‑specific: oral acyclovir, valacyclovir, or famciclovir for HSV and VZV; topical salicylic acid, cryotherapy, or immunomodulators for HPV warts; and curettage or cantharidin for molluscum. Supportive care—cool compresses, antihistamines, and moisturizers—relieves symptoms while the immune system clears the pathogen. Prompt dermatologic evaluation ensures accurate diagnosis, appropriate antiviral or procedural therapy, and education on contagion control.
Home Care and Natural Adjuncts for Mild Skin Infections
Evidence‑Based Home Remedies
| Remedy | Evidence Level | Typical Use | Safety/Precautions |
|---|---|---|---|
| Diluted tea‑tree oil (5 % in carrier) | Moderate (in‑vitro antimicrobial) | Apply 2‑3 times daily to mild bacterial lesions | Avoid undiluted oil; patch test for dermatitis |
| Medical‑grade honey (e.g., Manuka) | Moderate (wound healing) | Cover clean wound, change dressing daily | Not for deep or necrotic tissue |
| Apple‑cider‑vinegar rinse (1:1 with water) | Low (anionctic claim) | Gentle rinse 2 ×/day for fungal‑type patches | Rinse off; can irritate broken skin |
| Plain yogurt with live cultures | Low‑moderate (probiotic) | Apply as a paste for candidal rashes 2 ×/day | Discontinue if irritation occurs |
| Turmeric‑water paste (½ tsp turmeric in 2 tbsp water) | Low (anti‑inflammatory) | Apply to itchy fungal lesions 1 ×/day | Stains skin; wash off after 15 min |
| Warm moist compress | High (symptom relief) | 10‑15 min, 3‑4 ×/day for swelling | Ensure compress is not too hot |
Red‑flag signs (spreading redness, fever, increasing pain) → seek professional care.
 When over‑the‑counter (OTC) care is sufficient, mild bacterial infections can be managed by gently cleaning the area with mild soap and water, then applying an OTC topical antibiotic such as bacitracin or neomycin. Keep the site dry, protect it with a breathable bandage, and avoid scratching.
When over‑the‑counter (OTC) care is sufficient, mild bacterial infections can be managed by gently cleaning the area with mild soap and water, then applying an OTC topical antibiotic such as bacitracin or neomycin. Keep the site dry, protect it with a breathable bandage, and avoid scratching.
Safe home remedies and their evidence base: diluted tea‑tree oil (in a carrier oil), medical‑grade honey, or a mild apple‑cider‑vinegar solution may provide supplemental antimicrobial activity, while a warm, moist compress reduces swelling. For fungal‑type lesions, plain yogurt with live cultures or a turmeric‑water paste can offer anti‑inflammatory benefits. These measures are supportive but should not replace standard therapy.
Signs that home care is no longer enough: spreading redness, increasing pain, swelling, fever, or systemic symptoms indicate the need for professional evaluation and prescription antibiotics or antifungals. Prompt referral to a dermatologist ensures targeted treatment and prevents complications.
Skin Infection Nomenclature and Visual Guides
Visual Guide Summary
| Infection | Category | Visual Cue | Typical Treatment |
|---|---|---|---|
| Cellulitis | Bacterial | Diffuse erythema, warmth, swelling, poorly defined margins | Oral antibiotics (dicloxacillin, clindamycin) |
| Impetigo | Bacterial | Honey‑colored crusts, especially around mouth/nose | Topical mupirocin or oral cephalexin |
| Herpes Zoster | Viral | Unilateral vesicular rash following a dermatome | Oral valacyclovir 7‑10 days |
| HSV‑1/2 | Viral | Grouped vesicles on erythematous base; recurrent oral/genital lesions | Oral acyclovir/valacyclovir |
| HPV warts | Viral | Hyperkeratotic papules, often on hands/feet | Cryotherapy, salicylic acid, or imiquimod |
| Tinea corporis | Fungal | Ring‑shaped, erythematous, scaly border | Topical clotrimazole BID 2‑4 wks |
| Tinea pedis | Fungal | Interdigital maceration, peeling skin | Topical terbinafine 2‑4 wks |
| Candidiasis | Fungal | Red moist patches with satellite lesions | Topical nystatin or clotrimazole |
| Scabies | Parasitic | Burrow‑like linear lesions, intense itching at night | Topical permethrin 5 % |
| Molluscum contagiosum | Viral | Small smooth papules with central umbilication | Curettage or cantharidin |
Use the visual cues to quickly narrow differential diagnosis before confirming with lab tests.
 Skin infections encompass a broad spectrum: bacterial disorders such as cellulitis, impetigo, erysipelas, folliculitis, furunculosis, carbuncle, and staphylococcal or streptococcal infections; viral conditions like herpes simplex, herpes zoster (shingles), HPV warts, molluscum contagiosum, and varicella‑zoster; fungal illnesses including athlete’s foot (tinea pedis), ringworm (tinea corpore), jock‑itch (tinea cruris), candidiasis, and onychomycosis; and parasitic infestations such as scabies, lice, and Demodex. Common fungal infections present distinct visual patterns: tinea corpore appears as a red, circular, scaly patch with a raised border; tinea cruris shows a moist, itchy rash in the groin; tinea pedis features macerated, peeling skin between toes; tinea capitis causes patchy hair loss and scaly plaques; onychomycosis produces thickened, discolored nails; candidiasis manifests as red, moist patches with satellite lesions in skin folds. First‑line treatment for these superficial fungal infections is topical antifungal creams—clotrimazole, terbinafine, miconazole—applied once or twice daily for 2–4 weeks. Over‑the‑counter options (Lotrimin, Lamisil) are effective for mild cases, while prescription‑strength creams (ketoconazole 2%, ciclopirox) are reserved for persistent or extensive disease. If lesions do not improve, spread, or become painful, a dermatologist should evaluate the patient for possible oral therapy and a personalized preventive plan.
Skin infections encompass a broad spectrum: bacterial disorders such as cellulitis, impetigo, erysipelas, folliculitis, furunculosis, carbuncle, and staphylococcal or streptococcal infections; viral conditions like herpes simplex, herpes zoster (shingles), HPV warts, molluscum contagiosum, and varicella‑zoster; fungal illnesses including athlete’s foot (tinea pedis), ringworm (tinea corpore), jock‑itch (tinea cruris), candidiasis, and onychomycosis; and parasitic infestations such as scabies, lice, and Demodex. Common fungal infections present distinct visual patterns: tinea corpore appears as a red, circular, scaly patch with a raised border; tinea cruris shows a moist, itchy rash in the groin; tinea pedis features macerated, peeling skin between toes; tinea capitis causes patchy hair loss and scaly plaques; onychomycosis produces thickened, discolored nails; candidiasis manifests as red, moist patches with satellite lesions in skin folds. First‑line treatment for these superficial fungal infections is topical antifungal creams—clotrimazole, terbinafine, miconazole—applied once or twice daily for 2–4 weeks. Over‑the‑counter options (Lotrimin, Lamisil) are effective for mild cases, while prescription‑strength creams (ketoconazole 2%, ciclopirox) are reserved for persistent or extensive disease. If lesions do not improve, spread, or become painful, a dermatologist should evaluate the patient for possible oral therapy and a personalized preventive plan.
Personalized Dermatology Care at Dermatology Associates, PC
Diagnostic & Treatment Workflow at Dermatology Associates, PC
| Pathogen Type | Diagnostic Tool | Typical Findings | Tailored Treatment |
|---|---|---|---|
| Bacterial | Swab culture, Gram stain, PCR | Gram‑positive cocci clusters (Staph) or chains (Strep) | Topical mupirocin or oral dicloxacillin; MRSA‑covering agents (trimethoprim‑sulfamethoxazole) if needed |
| Fungal | KOH prep, fungal culture, PCR | Hyphae or yeast cells | Topical clotrimazole/terbinafine; oral terbinafine/itraconazole for extensive disease with LFT monitoring |
| Viral | PCR, Tzanck smear, viral culture | HSV DNA, VZV DNA | Oral acyclovir/valacyclovir; topical antiviral creams for HSV; lesion‑specific procedures for warts (cryotherapy) |
| Parasitic | Skin scraping, dermoscopy | Mites (scabies) or lice eggs | Topical permethrin 5 % or oral ivermectin |
Patient education includes hand hygiene, keeping skin dry, avoiding shared items, and staying up‑to‑date on vaccinations (shingles, HPV).
 Dermatology Associates, PC employs a full suite of diagnostic tools—skin swabs, cultures, KOH scrapings, PCR testing, and dermoscopy—to pinpoint bacterial, fungal, or viral pathogens before initiating therapy. Treatment plans are individualized: topical or systemic antibiotics for bacterial cellulitis, impetigo and MRSA; prescription‑strength antifungals (clotrimazole, terbinafine, oral itraconazole) for athlete’s foot, ringworm, candidiasis, and onychomycosis; and antivirals (acyclovir, valacyclovir, famciclovir) for herpes simplex, shingles and HPV-related warts. The practice emphasizes patient education on hand hygiene, keeping skin dry, avoiding shared items, and staying current with vaccinations such as shingles and HPV to reduce recurrence. Success stories include rapid resolution of recurrent tinea corporis after targeted oral terbinafine and a 90% reduction in HSV‑1 outbreaks with early valacyclovir, supported by scheduled follow‑up visits to monitor response and reinforce preventive habits.
Dermatology Associates, PC employs a full suite of diagnostic tools—skin swabs, cultures, KOH scrapings, PCR testing, and dermoscopy—to pinpoint bacterial, fungal, or viral pathogens before initiating therapy. Treatment plans are individualized: topical or systemic antibiotics for bacterial cellulitis, impetigo and MRSA; prescription‑strength antifungals (clotrimazole, terbinafine, oral itraconazole) for athlete’s foot, ringworm, candidiasis, and onychomycosis; and antivirals (acyclovir, valacyclovir, famciclovir) for herpes simplex, shingles and HPV-related warts. The practice emphasizes patient education on hand hygiene, keeping skin dry, avoiding shared items, and staying current with vaccinations such as shingles and HPV to reduce recurrence. Success stories include rapid resolution of recurrent tinea corporis after targeted oral terbinafine and a 90% reduction in HSV‑1 outbreaks with early valacyclovir, supported by scheduled follow‑up visits to monitor response and reinforce preventive habits.
Take Charge of Your Skin Health Today
Fungal skin infections—such as athlete’s foot, ringworm, jock itch, and candidiasis—typically appear as itchy, red, circular or scaly patches in warm, moist areas and require topical or oral antifungal therapy. Viral infections—including herpes simplex, shingles, warts, and molluscum contagiosum—present as vesicles, dome‑shaped bumps, or dermatomal rashes and are managed with antiviral drugs or procedural removal. See a dermatologist promptly if a rash spreads rapidly, becomes painful, is accompanied by fever, or does not improve with over‑the‑counter products. Dermatology Associates, PC offers board‑certified evaluation, skin scrapings or cultures for accurate diagnosis, personalized treatment plans (topical, oral, or procedural), and education on hygiene, dry‑skin practices, and vaccinations to prevent recurrence and protect long‑term skin health.
